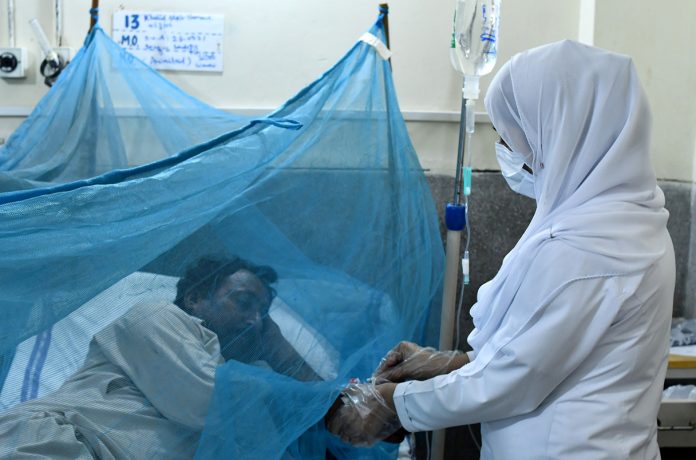
Relief may be in sight for tropical hospitals that are increasingly overwhelmed during outbreaks of dengue, a viral disease that can cause excruciating pain and even death. A new study has identified a compound that blocks dengue virus replication in test tube experiments and in mice, and it might one day be available as an easy-to-take pill.
If it works in clinical trials in humans, the drug could be given at primary care clinics, “which would be very important for the developing world where dengue is hyperendemic,” says Jenny Low, an infectious disease physician at Singapore General Hospital who was not involved in the work, reports Science.org.
Dengue, which is spread by mosquitoes that thrive in urban areas, annually infects more than 400 million people, primarily in Asia and Latin America. Most cases are mild, and patients recover on their own. But an estimated 96 million people come down with bad fevers, rashes, and muscle and joint aches that can last about a week. The disease is caused by four related viruses, or serotypes; subsequent infection with a different serotype increases the risk of internal bleeding and death. There are no drugs. During outbreaks, scores of patients with severe dengue rely on hospital care to manage the life-threatening symptoms.
The need to simultaneously protect against all four serotypes has stymied dengue vaccine development for decades. Finding a drug with balanced activity against all four was “like finding a needle in a haystack,” says Johan Neyts, a virologist at KU Leuven who led the study.
Starting in 2009, Neyts’s team screened tens of thousands of small molecules for antidengue activity using an automated high-throughput testing process. Chemists tweaked several molecules they found, producing more than 2000 compounds for further testing. One of those, named JNJ-A07, eventually proved equally potent against all four serotypes in test tube experiments. Next, the researchers administered the compound to mice, both before and after a dengue infection, to see whether the drug might be useful as a treatment, but also as a prophylactic. In both cases, the drug was “highly effective” in reducing viral loads and virus-induced disease, the team reports today in Nature.
The mouse results justify clinical trials for safety and efficacy in humans, says Cameron Simmons, an infectious disease scientist at Monash University, Clayton. But retired dengue researcher Scott Halstead, formerly of the Uniformed Services University of the Health Sciences, cautions against high expectations. “Experience has shown that the kind of in vitro data or even mouse model data cited here is not a reliable predictor of in vivo behavior,” he says.
Further lab work suggested JNJ-A07 blocks the functioning of the replication complex, an assembly of five proteins that interact to enable the dengue virus to copy itself inside cells. By shedding light on how the dengue replication proteins interact, Neyts’s work could lead to other drugs to treat the disease, says Eng Eong Ooi, a virologist at Duke-NUS Medical School in Singapore who was not involved in the study.
One apparent drawback is that for optimal effect, the drug would have to be given within a few days of symptom onset, before viral replication kicks into high gear. Many dengue patients don’t seek medical help until the third or fourth day of illness. “The therapeutic window to provide clinical benefits is very brief,” Simmons says.
“If you wait too long, it’s too late,” Neyts agrees. Deployment of the drug would need to be accompanied by educational campaigns for doctors and the public, he says. The drug could also be used as a prophylactic to blunt the impact of a community outbreak or by travelers visiting a dengue-endemic area, he says.
The drug is already in clinical trials, but Neyts declines to give details, saying scientists will present an update in November at the annual meeting of the American Society of Tropical Medicine & Hygiene. He also doesn’t want to hazard a guess as to when a drug might become available.
For clinicians, Low says, that moment can’t come soon enough: “The world has been searching for a direct-acting antiviral drug for decades.”