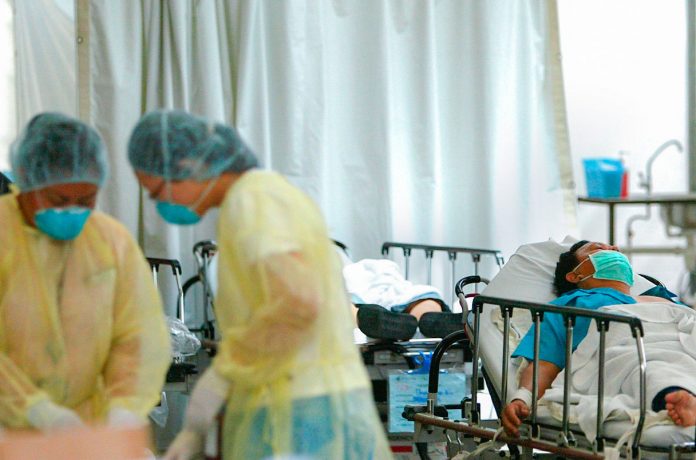
Almost 20 years before SARS-CoV-2, a related and even more lethal coronavirus sowed panic, killing nearly 10% of the 8000 people who became infected. But the 2003 outbreak of severe acute respiratory syndrome (SARS) may have left some survivors with a gift.
Former SARS patients who have been vaccinated against COVID-19 appear able to fend off all variants of SARS-CoV-2 in circulation, as well as ones that may soon emerge, a new study suggests, reports Sciencemag.org.
Their formidable antibodies may even protect against coronaviruses in other species that have yet to make the jump into humans—and may hold clues to how to make a so-called pancoronavirus vaccine that could forestall future outbreaks.
A team led by emerging disease specialist Linfa Wang from Duke-NUS Medical School in Singapore identified eight SARS survivors who recently received two shots of a messenger RNA COVID-19 vaccine.
In the test tube, antibodies sieved from their blood potently “neutralized” an early strain of SARS-CoV-2 as well as SARS-CoV, the virus that caused SARS, Wang and colleagues report today in The New England Journal of Medicine. The team further found these neutralizing antibodies worked well against the Alpha, Beta, and Delta variants of SARS-CoV-2 and stymied five related coronaviruses found in bats and pangolins that potentially could infect humans.
This study’s demonstration of broad spectrum immunity against sarbecoviruses—a subset of coronaviruses that includes the causes of SARS and COVID-19—is “amazing and very good news,” says Priyamvada Acharya, a structural biologist at Duke University who works on pancoronavirus vaccine research and was not involved in the new study.
“This paper provides a proof of principle that a pansarbecovirus vaccine is possible.” It also marks an important step toward a long-term hope—a vaccine that works against all coronaviruses—several researchers trying to develop this dreamed of protection say.
SARS-CoV and SARS-CoV-2 are about 80% identical, and both initiate infections when their surface protein, spike, binds to the human cellular receptor known as angiotensin-converting enzyme 2 (ACE2). So Wang was surprised this year when other researchers reported that people who had recovered from SARS retained antibodies that could prevent SARS-CoV from binding to the ACE2 receptor, but didn’t seem to have any power against SARS-CoV-2. “It was always in the back of my mind that the two viruses bind to the same receptor, so why don’t [these people’s antibodies] cross neutralize?” he wondered.
The immune system’s B cells make a potpourri of antibodies against any virus, but lab tests typically measure the presence of the most abundant ones. Maybe SARS survivors harbored a population of B cells that recognized both SARS-CoV and SARS-CoV-2 but were in the minority and difficult to see, Wang reasoned. If so, he thought, a COVID-19 vaccine might bolster the population of those double-action B cells—and broaden survivors’ immunity.
To test that possibility, Wang’s team compared neutralizing antibodies from the vaccinated SARS survivors—all health care workers in Singapore—with those from SARS patients who had not received a COVID-19 vaccine.
Wang’s team also analyzed antibodies in three other groups: unvaccinated people who currently had COVID-19, along with vaccinated people who had recovered from SARS-CoV-2 or had never been infected with that virus.
The vaccinated SARS survivors were the only cohort whose antibodies neutralized 10 different coronaviruses, according to a new assay Wang’s team developed that tests the antibodies’ ability to block binding between ACE2 and the receptor-binding domains (RBDs) of different spikes.
And the levels of the neutralizing antibodies were relatively high against each one. “It’s superinteresting,” says Neil King, a biomedical engineer at the University of Washington, Seattle, who is also working on pancoronavirus vaccines. “It may lead people to reprioritize their efforts.”
Several groups working on pancoronavirus vaccines are combining spikes or just the key RBDs from eight or more different viruses. But the new work suggests a combination of just two may be enough to reach a less ambitious goal, protecting against all sarbecoviruses. Then again, Wang has yet to identify why these antibodies work so well, which is critical to designing vaccines because the RBDs themselves likely will not trigger production of the wanted immune response.
The design of what are known as immunogens will require a complicated structural biology analysis, now underway in his group, that can determine precisely where they bind to the RBDs. That information, in turn, might allow researchers to reverse engineer the parts of spike that trigger production of these antibodies.
For a booster shot against possible SARS-CoV-2 variants or a pansarbecovirus vaccine, Wang suggests the best immunogens would combine common regions of SARS-CoV and the SARS-related viruses from pangolins and bats. “We want the vaccine to be as far away as possible from SARS-CoV-2, so that you really get the human immune system to work out only the common neutralizing antibody,” he says.
In parallel with the vaccine work, the lab has also isolated several individual antibodies from the COVID-19–vaccinated SARS survivors that are “much more potent” against SARS-CoV-2 than anything described by other groups. Made in quantity in the lab, those monoclonal antibodies could play a critical role in future outbreaks, Wang thinks.
“We are going to produce a cocktail of a dozen monoclonal antibodies that neutralize all the different sarbecoviruses and are ready to fight the next pandemic,” he says. “If we are unfortunate enough to have a SARS-3 down the line, we’ll already have a therapeutic cocktail ready to go.”
Andrew Ward, a structural biologist at Scripps Research who is developing pancoronavirus vaccines, calls the results from Wang’s team “pretty cool,” although he isn’t surprised that immunity to both SARS-CoV and SARS-CoV-2 may generate a broader sarbecovirus shield.
He is just as impressed that the study could even be done. Blood from the few SARS survivors is “a unique resource that that is hard to come by,” he says.
The combination of access to the SARS survivors in Singapore, which had the fifth highest number of cases of any country, and the new assay made this study possible, according to Wang. “No other lab could do this right now,” he says.